

search
date/time

Fri, 10:00PM
light rain
15.2°C
SSE 8mph
light rain
15.2°C
SSE 8mph
 | Sunrise | 3:36AM |
| Sunset | 8:29PM |  |
P.ublished 18th April 2026
lifestyle
Your Typical Doctor? Perhaps Not
Retired Cardiologist and author Liam Hughes writes for Yorkshire Times Newspapers about his life in medicine

Studying for medical finals or playing Scrabble?
The exams went better than expected especially in arts subjects and my A Levels picked themselves: Geography, History, Economics (a new subject said to be easy) and my banker, Maths because up until then no revision had been required.
I surfed in the slipstream of corporate excellence and although some were surprised by my A Level results, I wasn’t. Along with many others, I was encouraged to apply to Cambridge which meant an additional exam taken during an extra school term. The daunting prospect of another exam was mitigated by the possibility of gaining more representative sporting honours. The offered place produced disbelief in masters who had taught me during my early years and huge vicarious excitement by the PE staff who anticipated sporting Blues.
Life’s pristine lawn was laid out and I had another bonus. Despite the teeth, I had a girlfriend who was going to Oxford and so like me had nine months free before university. She suggested we go to South Africa together because her father remained there after the parental divorce. He was a budding politician in the newly formed Progressive Party and high up in the mining industry favoured by Marilyn Monroe. As the plane crossed the Equator, she announced that her first and true love was meeting us at the airport. Despite this unexpected setback her family were incredibly kind and generous especially when I was arrested for stealing the day’s takings from a famous Jo’burg off-licence chain. The police were surprised that a scruffy student was accompanied by the most senior legal advisor to the richest man in the world at that time.
Shortly after this, an initially dismissed doubt entered my head but it was unrelenting and within a few weeks, I was certain. Despite no family history of disease or medicine, I was going to be a doctor. I knew that with no science O Levels let alone A’s I couldn’t change my degree at Cambridge. My decision to decline the place caused some consternation except from my mother who quietly stated that she always knew I was going to study Medicine.

The former hospital porter is 2nd row, 3rd from left. 1973, Guy's intake
I wasn’t the most diligent medical student and learning biochemical pathways did not come easily. However, the most extraordinary metamorphosis happened after qualification. The academic knowledge of medical school was helpful but clinical medicine was all about experience and application, putting theory into practice, more akin to a trade apprenticeship. I found that the histories, test results and diagnoses of every patient were easy to recall. The registrars soon stopped betting whether I was bluffing or not when, without notes, I reeled off everything about the patient. I have subsequently realised that all of us can remember things that matter. Patients who declare that they are too stupid to understand their options - “so you decide doc” - can often take an engine apart, or recall every football team, or recite poetry.
From day one, I regularly received ‘golden nuggets’ from my fantastic consultant mentors, which starkly contrasts with the soul-destroying nature of a current foundation doctor’s roles. I learned that patients prefer to be seen by ‘their’ doctor or consultant, not whoever is on that shift and available. Continuity is also vital for formative medics. Receiving feedback on decisions and watching patients improve or not, is essential. Presenting patients to familiar seniors builds confidence and allows mentors to judge progress. I presented and received feedback on more than 1000 patients in my first year. Talking to current F1s they rarely have this opportunity.
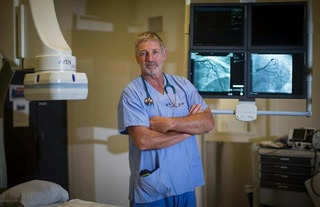
In the catheter lab where heart attacks are treated
After this fantastic year, despite what are now considered very long hours, I was hooked and wanted to be a hospital doctor. Although I enjoyed the day-case minor list during my surgical six months, becoming a physician was my aim. To achieve this, I would require another exam, Membership of the Royal College of Physicians (MRCP) which could be taken a few years after full registration. An 18-month Senior House Officer rotation at a distant hospital expanded my experience and I then returned to be the medical registrar under my previous boss and fortunately passed MRCP. Having celebrated this, another unheralded ambition hit me. My boss was a renowned gastroenterologist and we had discussed a possible career in the same speciality. When I announced that I wanted to be a cardiologist he wished me luck because the career pole was “greasy and studded with razor blades”, adding that an absence of multiple medical school prizes might make it difficult.
Determination is sometimes more important than talent. I became a cardiology research registrar. I published many papers including some based on my PhD research (a doctorate was almost mandatory to gain a consultant cardiology post). Ironically the doctorate had a significant biochemical component which I found easy because the science had direct clinical relevance. Luckily, I also came second in the British Cardiac Society’s Young Investigator award (young but by now 36), which is probably why I gained the now defunct level of Senior Registrar at St Bartholomew’s. I appreciate that competition for training posts in the UK is currently very tough but during the two years I was applying for this penultimate step to eventually becoming a consultant, only seven such posts were advertised in the whole UK.
Just after my fortieth birthday I commenced my consultant post at Royal Papworth and the Norfolk and Norwich hospitals. Over my time there, I helped develop cardiac services and although I trained in both the heart’s electrics and plumbing, the latter was my special interest. To improve local services, especially the immediate treatment of heart attacks by unblocking the offending artery as soon as possible, in 2007 I helped raise the £I.5 million NHS financial shortfall by rowing the Atlantic. Having seen the dire consequences of heart attacks before unblocking the culprit artery became the gold standard, it is no wonder that seeing gravely sick patients turn from grey to pink and leave hospital undamaged remained an addictive gratification until my retirement. The team buzz of salvaging patients was as, if not more, potent, than snatching victory from defeat on the sporting fields of my youth.

My new job
More information here: https://www.eye-books.com/products/bodily-fluids
Read our review of Bodily Fluids here: Blood, Bile, Pus: Bodily Fluids By Liam Hughes

